Source: The Conversation – Canada – By Habib Rezanejad, Professor of cellular and molecular biology, MacEwan University
As a researcher, I still remember the discomfort I felt every time I had to sacrifice laboratory animals for an experiment. For decades, animals like mice, rats and pigs have been essential tools in biomedical research. Yet many scientists are asking whether better, more humane alternatives are possible.
Globally, it’s estimated that close to 200 million animals are used in laboratory research each year. While animal models have helped generate major medical breakthroughs, they don’t always reflect how human biology works.
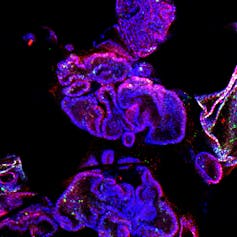
(Habib Rezanejad)
New technologies are now offering scientists a promising alternative: organoids — tiny three-dimensional versions of human organs grown in the lab.
These “mini organs” are grown from human stem cells and can reproduce some of the complex cell types and interactions found in the body. Because they’re derived from human cells, organoids offer researchers a way to study human diseases more directly than traditional animal models.
Organoids for brain research
This approach is gaining huge attention in brain research. Compared with many other organs, the brain presents unique challenges for scientists.
Brain disorders are often complex and difficult to define precisely, involving subtle changes across many types of cells and neural circuits. At the same time, the brain is one of the least accessible organs in the body. Unlike blood or skin, living brain tissue cannot be easily sampled from healthy individuals.
Alzheimer’s disease, for example, is a growing global health concern, especially as populations age. Yet finding treatments has proven extremely difficult. A systematic review of research over two decades found that 98 Alzheimer’s drug candidates failed in clinical trials while only two succeeded. This highlights the enormous challenge of developing effective therapies.
One reason for this failure is that drugs that work in animals often do not work in humans. Mice and humans share many biological features, but important species differences mean animal models cannot fully reproduce the architecture and complexity of the human brain.
Traditional laboratory models also have other limitations. For example, many experiments rely on two-dimensional cell cultures, where cells grow in flat layers on plastic dishes. While useful, these systems lack the three-dimensional structure and cell-to-cell interactions found in real tissues. Without that complexity, they cannot accurately mimic many disease processes.
This is where organoids are transforming biomedical research.
In 2013, scientists demonstrated that brain organoids grown from human stem cells can self-organize into structures resembling parts of the developing brain. These “mini brains” contain multiple neural cell types and can mimic aspects of early brain development.
Researchers now use them to study conditions like autism, Alzheimer’s disease and amyotrophic lateral sclerosis (ALS).
Intestine, liver, kidney, pancreas
Beyond the brain, scientists have created organoids that resemble many other tissues, including the intestine, liver, kidney and pancreas.
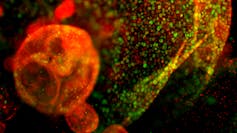
(Habib Rezanejad)
These models allow researchers to study diseases and test chemicals on human-like tissues rather than animals. For example, organoids could one day be used to screen chemicals for toxicity across multiple organs using cells derived from different individuals.
In my own research, my lab grows organoids from human and mouse pancreatic tissue to study cellular diversity and pancreatic inflammation. These models allow us to explore how different pancreatic cell types behave in three dimensions — something that would be impossible to observe in traditional flat cell cultures.
Potential for personalized medicine
A key advantage of organoids is their ability to capture human diversity. Laboratory mice used in experiments, on the other hand, are often genetically identical, which does not reflect the diversity of human populations.
Organoids can be grown from cells donated by individual patients, allowing researchers to study how diseases develop in different genetic backgrounds.
This opens the door to personalized medicine, where scientists test potential treatments on patient-derived organoids before giving them to patients.
Patient-derived organoids can predict how individuals might respond to certain drugs — for instance, responses to chemotherapy in metastatic colorectal cancer patients.
Organoids grown from many individuals, on the other hand, may provide a more realistic representation of how a population will respond to drugs. This helps researchers identify treatments that are more likely to succeed in clinical trials.
Overall, organoids are becoming powerful tools for drug discovery and safety testing.
Could this be the end of animal testing?
Some scientists believe organoids may replace animals altogether in certain areas of research. Organoid technology aligns with the “3Rs” principles in animal research — reduction, refinement and replacement — that aim to minimize the use of animals in science.
Reflecting this shift, the United States National Institutes of Health (NIH) recently announced it will prioritize research technologies that use human-based models rather than relying solely on animal experiments.
Pioneers in the field are optimistic. Hans Clevers, a leading scientist who helped develop gut organoids, has suggested that organoids could eventually replace animals in some forms of toxicology testing within the next few decades.
Still, organoids are not perfect
Although they are far more complex than traditional cell cultures, organoids remain simplified versions of real organs. Many lack blood vessels, which limits their size and maturity. They do not yet capture the full diversity of cell types found in human tissues, such as immune cells.
Studies have also shown that cells within organoids can experience stress due to laboratory growth conditions.
For now, organoids should be seen as powerful additions to the scientific toolbox rather than complete replacements for animal models.
Organoids are still an emerging technology, but they are already reshaping how scientists study human biology and disease. As the technology improves, these tiny lab-grown organs may help researchers reduce reliance on animal testing while bringing us closer to understanding — and treating — complex human diseases.
![]()
Habib Rezanejad receives Alberta Innovates Summer Research Studentship from Alberta Innovates for a research project at MacEwan University in 2025.
– ref. Can ‘mini brains’ replace lab animals? Organoids are changing how scientists study disease – https://theconversation.com/can-mini-brains-replace-lab-animals-organoids-are-changing-how-scientists-study-disease-277611
